Stress Incontinence in Women

Stress incontinence is an embarrassing condition which is very common in women. According to a USA study between 2015-2018 (1), it was found that 61.8% of the women in the study were affected by incontinence at least once a month. Of this percentage 37.5% complained of stress incontinence and a further 31% had mixed stress and urge incontinence.
Incontinence can hamper the way you play sports or your choice of physical activity, as pressure while jumping, sprinting is one of the biggest stresses that occur when you have stress incontinence.
What is Stress Incontinence?
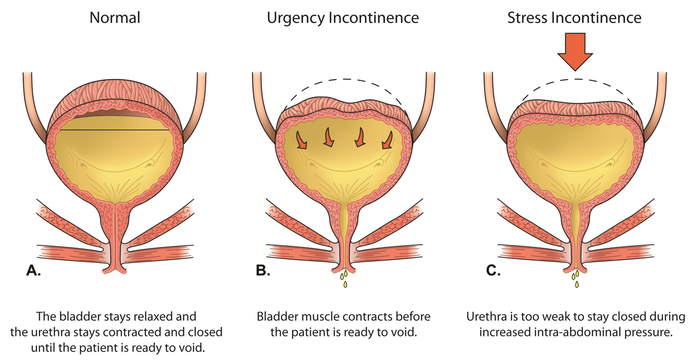
Image courtesy of Northwestern Medicine
Stress incontinence is urine leakage which occurs when the muscles and other tissues that support the urethra (pelvic floor muscles) and the muscles that control the release of urine (urinary sphincter) weaken.
Stress incontinence usually occurs during exercise, coughing, sneezing, laughing, and other body movements that put pressure on the bladder.
Typically, valve-like muscles in the urethra stay closed as the bladder expands, preventing urine leakage until you reach a bathroom. But when those muscles weaken, anything that exerts force on the abdominal and pelvic muscles can put pressure on your bladder and cause urine leakage.
Why Do The Muscles and Sphincter Weaken?
Some of the known causes include:
● Injury to the urethra or surrounding areas
● Childbirth, tissue or nerve damage during childbirth can weaken the pelvic floor or the sphincter, either directly after child birth or years later.
● Pelvic Prolapse
● Some medicines
● Surgery in the pelvic area (hysterectomy)
● Being overweight
Factors That Lead To Stress incontinence
● Illnesses that cause chronic coughing
● Obesity
● Smoking, which can cause frequent coughing
● High-impact activities, such as running and jumping, over many years
● Age
When Does Stress Incontinence Occur?
When either set of muscles become weak, urine can pass when pressure is placed on your bladder. You may notice it when you cough, sneeze, laugh, exercise, lift heavy objects or engage in sexual activity.
What Can You Do To Manage Stress Incontinence?
1. Behavioral Therapy
You can change your lifestyle and the way you live to reduce episodes of stress incontinence.
● If you’re obese, your doctor may advise you to lose weight.
● You might also try to avoid activities that cause leakage, such as jumping or jogging.
● Nicotine can irritate your bladder and may contribute to incontinence. If you are a smoker, it is advised to quit the habit. The constant cough seen in smokers also contributes to the problem.
● Lastly, consider avoiding caffeine and alcohol, as these substances cause diuresis which increases fluid volume in the bladder. You might want to cut back on your overall fluid intake to reduce bladder pressure.
2. Pelvic Muscle Training
Kegel exercises make your sphincter and pelvic muscles stronger. When learning to perform kegels, contract the muscles you use to stop a stream of urine. It can initially be helpful to practice doing kegels on the toilet to help you learn which muscles to use. But only initially, do not continue to always stop mid flow as it may impair your bladder emptying in the long run. Once you have mastered which muscles to use, you can perform kegels anywhere at anytime.
Electrical stimulation is another treatment, and it sends a mild electrical current through your pelvic floor muscles. The current makes your muscles contract, mimicking a Kegel exercise. You may be able to contract the muscles yourself after feeling exactly which muscles are contracting. ● Using vaginal weights while exercising to strengthen the pelvic floor.
Using vaginal weights while exercising to strengthen the pelvic floor.
3. Purpose-Made Devices
These are products designed specifically to reduce stress urinary incontinence (SUI).
Intravaginal Bladder Support:
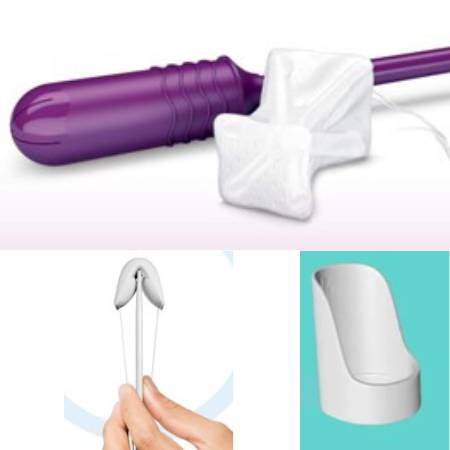
This is inserted into the vagina by the user herself using an applicator much like a normal tampon applicator. The device features soft nylon mesh stretched over a shaped silicone core, which expands after the applicator is withdrawn to provide support to the urethra in order to prevent incontinence. This is a single-use, disposable over-the-counter product available in a range of sizes.
Intravaginal Ring: these are re-usable bladder neck support prosthesis which are inserted and removed by the user each day.
When do internal vaginal devices work best?
Internal vaginal devices are intended for use during normal everyday activities. While the devices work well for some women, for others they do not. Most effective for women with minimal to moderate SUI leakage. Intravaginal rings have been found to be less effective in women with mixed urinary incontinence.
Any internal device can cause discomfort or irritation so that it may be best to limit their use to times when wearing a pad may be less convenient. Most suitable for use intermittently to provide occasional continence protection during physical activities such as exercising or dancing. The intravaginal bladder support is intended to be used only for up to twelve hours in any twenty-four-hour period.
4. Medication
Both oral and topical oestrogen supplements may help in women. Sometimes, pseudoephedrine is used with success.
5. Surgery
If you have a severe case of stress incontinence, to the point that it interferes with your everyday life, your doctor may recommend surgery. Several types of procedures are available and include vaginal repairs and slings to lift the bladder and urethra. During the surgery, doctors will try to provide your urethra and bladder with more support.
- A sling procedure uses your own tissues to create a support structure for the urethra.
- A tension-free sling is a mesh usually made from a synthetic material called polypropylene. To support the urethra, the sling functions like a hammock and is held in place by body tissues rather than stitches. During the healing process, scar tissue forms in and around the mesh to keep it from moving.
Physiotherapy Treatment for Stress Incontinence
There is no need to suffer the embarrassing consequences of incontinence in silence. There are many ways to treat stress incontinence, depending on the severity or cause of your condition. If you experience urine leakage while moving or exercising, see your doctor for a referral to physiotherapists today.
Need Help? Contact Us Today
At Prohealth Sports & Spinal Physiotherapy Centres, we offer treatments for stress incontinence, urinary incontinence, as well as other women’s health conditions and musculoskeletal injuries.
Our team of physiotherapists are professional and experienced in working with clients with women's health-related conditions. At Prohealth Sports And Spinal, we always strive to give the highest standard of physical therapy and care to help our clients achieve the best possible outcomes.
Our treatment plans are always personalised for each individual to each their maximum recovery potential.
If you would like an assessment, reach out to our physiotherapists who can help you and advice on any specific exercises.
For more information, contact us at +852 2530 0073, or email appt@sportsandspinal.hk.
Written By: Mel Potgieter
BPHYST (University of Pretoria, South Africa)
HKNA Elite Programme Physiotherapy Partner
Mel is an experienced physiotherapist based out of the Prohealth Sports And Spinal Physiotherapy Centre on Wellington Street, Central. She is an expert in pelvic dysfunction, back pain, getting the core going after pregnancy, post-mastectomy and abdominal /cosmetic surgeries, lymph drainage for cancer patients, as well as acute sports injuries and post surgery rehabilitation.
Outside of the clinic, she is a formidable netball player and is active in the Hong Kong Netball Association.